I. Nhanganyaya
Iyo distal humerus inoumbwa nepakati uye lateral columns, iyo inosanganisira epicondyles uye condyles.
II. Kuvhiya Maitiro
Distal humerus fractures inokonzerwa nekukuvara kwakananga (semuenzaniso, kudonha) kana masimba asina kunanga (semuenzaniso, kumonyoroka kana kudhonza tsandanyama).
III. Post-op Rehabilitation
The AO classification inokamura distal humerus fractures mumhando nhatu huru: A , B , uye C .
IV. Zvidzidzo zvekudzidza
Kurapa kwekuvhiya kunotevera misimboti yeAO: kuderedzwa kweanatomical, kugadzirisa kwakagadzikana, uye kugadziridza kwekutanga.
V. Nyaya Yenyaya
Kukiya mahwendefa anopa yepamusoro biomechanical kugadzikana, kunyanya mune osteoporotic bone.
VI. Kukurukurirana
CZMEDITECH inopa mhando nhatu: extraarticular (01.1107), lateral (5100-17), uye medial (5100-18) mahwendefa.
VII. Mhedziso
Kurapa kwekuvhiya kunotevera misimboti yeAO: kuderedzwa kweanatomical, kugadzirisa kwakagadzikana, uye kugadziridza kwekutanga.
Distal tibial fractures inowanzoitika, uye marapirwo echinyakare ane miganhu
Distal tibial fractures imhando yakajairika yekuputsika kwegumbo rezasi. Mishonga yechinyakare senge maplate ekukiya uye antegrade intramedullary mbambo imwe neimwe ine zvayakaipira. Kukiya mahwendefa kunogona kukonzera postoperative zvirwere kana soft tissue necrosis, kuwedzera kupora; kunyange zvazvo zvipikiri zveantegrade zvisinganyanyi kupindira, zvinogona kukuvadza majoini emabvi, kukonzera marwadzo, uye kutakura njodzi dzekugadzirisa kusina kukwana kana kukanganisa, kutadzisa kupora.
Locking plates:
Yakakosha kukuvara kwenyama yakapfava, huwandu hwehutachiona hwepamusoro, kupora kwenguva refu
Antegrade misumari:
Ngozi yekukuvara kwemabvi akabatanidzwa, kugadzirisa kusina kukwana, kunowanzoita malalignment
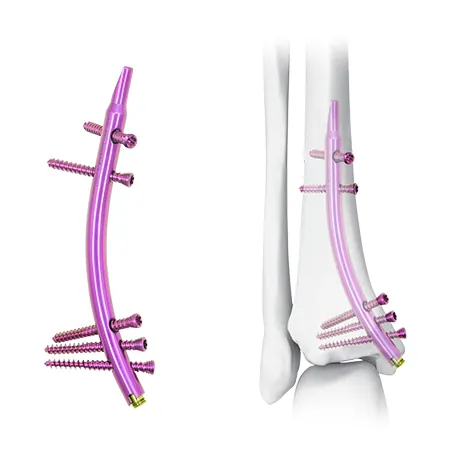
Mhinduro nyowani: Distal Tibial Nail (DTN)
Iyo itsva yekurapa sarudzo-Distal Tibial Nail (DTN)-inopa maonero matsva ekugadzirisa distal tibial fractures neyakasiyana yekudzoreredza dhizaini.
Retrograde yekuisa dhizaini inopa nzira nyowani

Kuiswa kwemurwere uye kuderedza kugadzirira
Murwere anoiswa panzvimbo yepamusoro. Displaced fractures inofanira kuderedzwa nemaoko; kana zvichidikanwa, shandisa reduction forceps kubatsira usati waisa iyo DTN. Kana paine kufambidzana kwefibular fracture, kurongeka kwakakodzera kwefibula kunogona kubatsira kuderedza tibial. Fibular shaft fractures inogona kugadzika ne intramedullary misumari. Nokuda kwekuputsika kwakapoteredza chitsitsinho, kuderedzwa kweanatomical uye kugadziriswa kwefibula kunofanira kutangira kuderedzwa kwetibial kudzivirira kusarura. Mukuvhurika mafractures ane aripo ekunze fixation, mbambo inogona kuiswa ichichengetedza iyo fixator kuti iwane kuderedza.
Supine chinzvimbo, shandisa kuderedza forceps kana zvichidikanwa
Isa pamberi fibular fracture manejimendi kuti uve nechokwadi chekudzikisa tibial
A 2-3 cm longitudinal incision inoitwa pamuromo wemedial malleolus kuburitsa pachena deltoid ligament. Pini yemutungamiri inoiswa kana kuti zvishoma zvishoma kusvika kumucheto we malleolus (Fig. 2a), 4-5 mm kubva kune articular surface. Maonero ekupedzisira anoratidza kuiswa kuburikidza ne intercondylar groove (Fig. 2b), kudzivisa kukanganisa kune posterior tibialis muscle. Kuparadzanisa iyo yepamusoro deltoid ligament, zvino shandisa reamer kuti ukure medullary canal kusvika kune metaphyseal region (Fig. 2c). Bvisa cancellous bone pedyo neproximal medial cortex kuti uise mbambo (Fig. 2d). Isai mbambo yekuedza kusimbisa hukuru hweDTN (Fig. 2e). Dzivisa kusando kana kumonyoroka zvakanyanya kudzivirira iatrogenic medial malleolar fracture. Rongedza kudzika kwembambo kuti ive nechokwadi chekuti distal screws haipinde mujoini yezviziso kana nzvimbo yekutyoka. Kugadziriswa kunowanikwa neakavharira screws proximally uye disally.
Incision:
Longitudinal yakachekwa pane medial malleolus tip
Pini yekumisikidza:
4-5 mm kubva pajojo pamusoro
Kuongorora & kuedza chipikiri:
Ream kusvika kune metaphysis, simbisa saizi yembambo
Kuisa chipikiri:
Dzivisa kusando, gadzirisa kudzika kuchengetedza majoini
Kugadzirisa:
Interlocking screws proximally uye disally
Nzira yekuisa DTN





Pakarepo majoini ekufamba-famba uye kutsika-pasi-pasi kunobvumirwa mushure mekushanda
Kusina uremu kutakura kwemavhiki e4-6
Kufambira mberi kusvika kuzere uremu pakati pevhiki 8-12, uchitarisa kuumbwa kwe callus uye kurwadziwa.Ankle joint basa rinotanga pakarepo mushure mekuvhiyiwa
Dzivisa kurema kwemavhiki 4-6
Zvishoma nezvishoma shanduko kusvika kuzere uremu-kubereka pamavhiki 8-12
Kutevera kwevarwere gumi
Chidzidzo chakatevera varwere ve10 (Tafura 1). Pakazosvika 3 months post-op, 7 nyaya dzakanga dzapora; varwere vese vakawana kuporeswa mukati memwedzi mitanhatu. Imwe nyaya imwe neimwe yevarus uye recurvatum deformities yakaitika. Hapana kurasikirwa kwekuderedza, hutachiona, matambudziko ane chokuita nekudyara, kana kukuvara kweatrogenic kwakaonekwa (Tafura 2).
7 kesi dzakaporeswa mukati memwedzi mitatu; vose vakaporeswa nemwedzi mitanhatu
2 zvinyoro zvirema (1 varus, 1 recurvatum)
Hapana hutachiona, matambudziko ekudyara, kana kurasikirwa kwekuderera


Murwere ane makore 69 okuberekwa
Mhando yekutsemuka:
Transverse tibial fracture + fibular fracture
Dambudziko:
Soft tishu kupwanya kukuvara
Post-op:
6 chete diki incisions, kupora kwakakwana mukati me1 gore
Zvifananidzo 3 & 4:
Radiographic uye postoperative kupora mifananidzo







Zviratidzo zveDTN
Ichi chidzidzo chaisanganisira AO 43-A uye C1 fractures; C2 yakaonekwawo. DTNs inowanikwa muhurefu hwe 7 mm uye 8 mm, iyo inosarudza kuiswa kweproximal interlocking screws. Mafractures anowanikwa 2-9 cm pamusoro peiyo articular surface akakodzera kukwikwidza DTN kugadzirisa. Zviratidzo zvinogona kuwedzera kusvika kuAO 42 fractures.
Inoshanda kuAO 43-A, C1, funga kuwedzera kuC2 uye 42
Mhedzisiro yakanakisa yekutyoka 2-9 masendimita kubva pajoint surface
Biomechanical Kugadzikana
Retrograde misumari ine yepamusoro axial uye inotenderera kuoma kana ichienzaniswa neyemukati yekukiya mahwendefa uye antegrade zvipikiri. Greenfield et al. yakaita biomechanical test kuratidza kuti kushandisa distal screws muDTN kwakawana 60–70% yekuomarara kwakasimba uye 90% yekuomarara kwepamuviri zvichienzaniswa nemasruuru matatu. DTN yakaderedza fracture fragment kufamba pasi pemutoro. Muzviitiko zvitatu zvisina kupora mukati memwedzi ye3, zvinhu zvaisanganisira kukuvadzwa kwenyama yakapfava, kuwedzera kwe medullary, nzvimbo yekutyoka, uye osteoporosis. Sezvo maDTNs achiuya nemasaizi matatu chete uye distal fixation inogumira kune matatu screws, anogona kupa kusakwana kugadzikana mumigero yakakura kana osteoporotic bone. Kuremera kwekutanga kunofanira kusvikirwa nekuchenjerera mumamiriro ezvinhu akadaro.
Yakakwirira kukiya mahwendefa uye antegrade zvipikiri
Yakakurudzirwa kugadzirisa zano: 2 proximal + 3 distal screws
Zvakanakira zveDTN
Zvichienzaniswa nekuvhara mahwendefa, intramedullary misumari inokonzeresa kushomeka kwematishu akapfava, kunyanya akakodzera kuvarwere vakura uye avo vane kukuvara kwakanyanya kwenyama yakapfava kubva mukukuvadzwa kukuru kwesimba. Muchidzidzo ichi, maDTNs akaiswa kuburikidza nediki diki nhanhatu, pasina matambudziko akapfava. Iyo nzira haidi kuchinjika kwebvi, kuderedza njodzi yekuderedza kurasikirwa uye kuita kuti ive yakakodzera kune varwere vane mabvi mashoma kufamba (semuenzaniso, mabvi arthritis kana post-TKA).
Minimally invasive, yakanakira vakwegura uye high-energy trauma varwere
Hapana kuchinjika kwebvi kunodiwa, kwakakodzera kufamba kwemabvi mashoma
Kuvhiya Njodzi uye Chengetedzo
Ngozi dzinosanganisira kukuvara kune posterior tibialis muscle uye medial malleolar fracture. Medial malleolar fractures inogona kurapwa netension band wiring, plating, kana kunze kwekugadzirisa.
Kuchengetedza kunofanira kutorwa kudzivirira kupinza screw mufibular notch. Iyo yekumisikidza mudziyo inogona kukonzera kumashure kutenderera kweDTN nekuda kwehuremu hwayo; gadzirisa screw yechipiri kunongedza kune fibula (Fig. 4c).Zvinetso zvinogona kuitika:
Posterior tibialis kukuvara, medial malleolar fracture
Management:
Tension bhendi, plating, kana yekunze fixator
Screw direction uye positioning device uremu zvinoda intraoperative attention
Clinical Kuenzanisa
Izvo zvisizvo uye mazinga ekukanganisa kwezvipikiri zveantegrade ndeye 0-25% uye 8.3-50%, zvichienderana; yekuvhara mahwendefa, 0-17% uye 0-17%. Muchidzidzo ichi, zviitiko zvose zvakawana kubatana, uye 20% chete yakanga ine urema> 5 °, inofananidzwa nemaitiro echinyakare.Matanho ehutachiona: hutachiona hwepamusoro ndeye 0-8.3% yezvipikiri zve antegrade uye 0-23% yekuvhara mahwendefa; hutachiwana hwakadzika huri 0-23% uye 0-8.3%, maererano. Chidzidzo ichi chakashuma kuti hapana matambudziko ematishu akapfava, achikunda dzimwe nzira dzese.Functional scores:
AOFAS zvibodzwa zveantegrade misumari: 86-88 (rudzi A), 73 (rudzi C); kukiya ndiro: 84–88 (rudzi A)
Ichi chidzidzo: AOFAS avhareji: 92.6
EQ-5D-5L: Kuvhara mahwendefa: 0.62-0.76; chidzidzo ichi: 0.876
SAFE-Q (varwere vetsoka nemakumbo): 67-75; chidzidzo ichi: 83–91.7 (Tafura 3)
Mwero wemubatanidzwa, deformity rate, uye huwandu hwehutachiona hunokunda nzira dzechinyakare
Zvibodzwa zvinoshanda (AOFAS, EQ-5D-5L, SAFE-Q) zvinoratidza mhedzisiro yakanaka

Muchidimbu, DTN inopa zvakanakira pamusoro pekuvhara mahwendefa uye antegrade intramedullary zvipikiri uye inomiririra mhinduro inoshanda yekurapa distal tibial fractures.
DTN inoratidzira kushomeka kwekupinda, kugadzikana kwakanyanya, uye nekukurumidza kupora
Iyo yakakosha kune mamwe marapirwo echinyakare uye akakodzera kusimudzira