Kyphoplasty Balloon Vertebral Perforator: A Breakthrough Treatment for Vertebral Compression Fractures
Introduction
Vertebral compression fractures (VCFs) are a common condition, especially in the elderly population, and are often associated with osteoporosis. Traditional treatments for VCFs include conservative management, such as pain medication and bracing, or surgical interventions such as spinal fusion. However, these treatments may have limited efficacy or lead to other complications. Kyphoplasty balloon vertebral perforator (KBP) is a minimally invasive, breakthrough treatment for VCFs that has revolutionized the management of this condition. In this article, we will explore the mechanism, indications, benefits, and risks associated with KBP.
Anatomy and Mechanism of VCFs
VCFs occur when the vertebral body collapses due to weakened bone structure, often caused by osteoporosis or trauma. The vertebral body is the central portion of the vertebra, and is composed of cancellous bone surrounded by a thin layer of cortical bone. When the vertebral body collapses, it can result in significant pain and disability.
Indications for Kyphoplasty Balloon Vertebral Perforator
KBP is indicated for the treatment of painful VCFs that have failed to respond to conservative management, or in cases where surgery is not a suitable option. The procedure is generally well-tolerated and has a low risk of complications.
The Kyphoplasty Balloon Vertebral Perforator Procedure
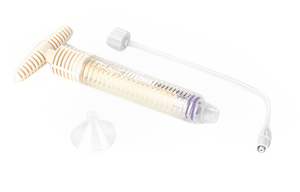
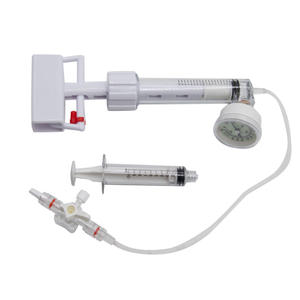
KBP involves the use of a small balloon catheter that is inserted into the collapsed vertebral body under fluoroscopic guidance. The balloon is then inflated to restore the height of the vertebral body and create a cavity. Once the cavity is created, bone cement is injected to stabilize the vertebral body and prevent further collapse.
Advantages of Kyphoplasty Balloon Vertebral Perforator
KBP has several advantages over traditional treatments for VCFs. Firstly, it is a minimally invasive procedure that can be performed under local anesthesia, reducing the risks associated with general anesthesia. Secondly, it is associated with a shorter hospital stay and quicker recovery time compared to traditional surgery. Finally, KBP has a high success rate, with most patients experiencing significant pain relief and improved function following the procedure.
Risks and Complications of Kyphoplasty Balloon Vertebral Perforator
Like any medical procedure, KBP carries some risks and potential complications. These may include infection, bleeding, nerve damage, cement leakage, or worsening of the fracture. However, the risk of these complications is relatively low, and most patients tolerate the procedure well.
Post-Procedure Care and Rehabilitation
After KBP, patients are typically monitored for a short period and can usually return home the same day. They are advised to avoid heavy lifting and strenuous activity for several weeks, but can typically resume normal daily activities within a few days. Physical therapy may also be recommended to help with rehabilitation.
Future Directions for Kyphoplasty Balloon Vertebral Perforator
KBP is a relatively new procedure, and ongoing research is exploring its potential applications and refinements. For example, there is ongoing research into the use of biodegradable bone cement, which could reduce the risk of long-term complications associated with traditional cement.
Conclusion
Kyphoplasty balloon vertebral perforator is a minimally invasive, breakthrough treatment for painful VCFs that has revolutionized the management of this condition. The procedure is generally well-tolerated and has a high success rate, with most patients experiencing significant pain relief and improved function following the procedure. While there are some risks associated with the procedure, these are generally low, and most patients tolerate the procedure well. As ongoing research explores the potential applications and refinements of KBP, this procedure is likely to continue to be an important tool in the management of VCFs.
FAQs
Is KBP a suitable treatment option for all patients with VCFs?
KBP is indicated for the treatment of painful VCFs that have failed to respond to conservative management or in cases where surgery is not a suitable option. However, not all patients with VCFs are candidates for KBP, and the decision to undergo the procedure should be made in consultation with a healthcare provider.
How long does the KBP procedure take?
The KBP procedure typically takes around one hour to perform.
How soon after the procedure can patients resume normal activities?
Patients can typically resume normal daily activities within a few days after the procedure, although heavy lifting and strenuous activity should be avoided for several weeks.
What are the potential complications associated with KBP?
Potential complications associated with KBP may include infection, bleeding, nerve damage, cement leakage, or worsening of the fracture. However, the risk of these complications is generally low.
Is KBP covered by insurance?
KBP is usually covered by insurance, although coverage may vary depending on the patient's individual insurance plan and other factors.
Español
Русский
Français
English
العربية
Português
Deutsch
italiano
日本語
한국어
Nederlands
Tiếng Việt
ไทย
Polski
Türkçe
አማርኛ
ພາສາລາວ
ភាសាខ្មែរ
Bahasa Melayu
ဗမာစာ
தமிழ்
Filipino
Bahasa Indonesia
magyar
Română
Čeština
Монгол
қазақ
Српски
हिन्दी
فارسی
Kiswahili
Slovenčina
Slovenščina
Norsk
Svenska
українська
Ελληνικά
Suomi
Հայերեն
עברית
Latine
Dansk
اردو
Shqip
বাংলা
Hrvatski
Afrikaans
Gaeilge
Eesti keel
Māori
नेपाली
Oʻzbekcha
latviešu
অসমীয়া
Aymara
Azərbaycan dili
Bamanankan
Euskara
Беларуская мова
भोजपुरी
Bosanski
Български
Català
Cebuano
Corsu
ދިވެހި
डोग्रिड ने दी
Esperanto
Eʋegbe
Frysk
Galego
ქართული
guarani
ગુજરાતી
Kreyòl ayisyen
Hausa
ʻŌlelo Hawaiʻi
Hmoob
íslenska
Igbo
Ilocano
Basa Jawa
ಕನ್ನಡ
Kinyarwanda
गोंगेन हें नांव
Krio we dɛn kɔl Krio
Kurdî
Kurdî
Кыргызча
Lingala
Lietuvių
Oluganda
Lëtzebuergesch
Македонски
मैथिली
Malagasy
മലയാളം
Malti
मराठी
ꯃꯦꯇꯥꯏ (ꯃꯅꯤꯄꯨꯔꯤ) ꯴.
Mizo tawng
Chichewa
ଓଡ଼ିଆ
Afaan Oromoo
پښتو
ਪੰਜਾਬੀ
Runasimi
Gagana Samoa
संस्कृत
Gaelo Albannach
Sepeti
Sesotho
chiShona
سنڌي
Soomaali
Basa Sunda
Wikang Tagalog
Тоҷикӣ
Татарча
తెలుగు
ትግንያውያን
Xitsonga
Türkmençe
संस्कृत
ئۇيغۇرچە
Cymraeg
isiXhosa
ייִדיש
Yorùbá
isiZulu