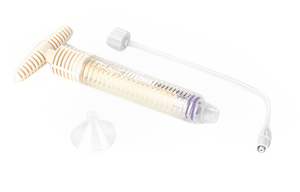
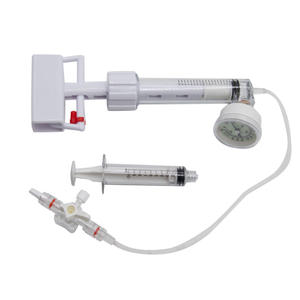
A variety of extra-arch puncture methods have been successfully used for percutaneous vertebroplasty (PVP) and percutaneous kyphoplasty (PKP).
Percutaneous vertebroplasty (PVP)
Percutaneous vertebroplasty (PVP) is a treatment for patients with one or more symptomatic vertebral fractures caused by bone tumors, osteoporosis or trauma. In PVP, a bone biopsy needle is inserted into the fractured vertebrae under local anesthesia in the patient; a bone cement made of polymethylmethacrylate (PMMA) is injected through the needle, followed by immediate relief of symptoms such as difficulty walking or low back pain . A single PVP procedure requires only 2 hours of treatment time and 2 hours of postoperative bed rest; it can be performed through a 5-mm skin incision for insertion of each bone biopsy needle, it has a low incidence of serious adverse events, can be performed without special preoperative preparation or intensive postoperative care, and the only absolute contraindications are uncontrollable infection and bleeding tendencies.PVP, as a minimally invasive procedure, has a low complication rate It is also characterized by the fact that patients can go home after treatment without hospitalization and can treat elderly patients over 90 years of age with guaranteed outcomes.
Percutaneous kyphoplasty (PKP)
Percutaneous kyphoplasty (PKP) is currently an effective and widely used treatment for osteoporotic vertebral compression fractures (OVCF), which is usually performed under local anesthesia and is well tolerated by patients. Early studies have shown promising clinical outcomes in terms of immediate pain relief and improved function, especially in the elderly. However, there is still a very high number of patients who are not satisfied with the post-surgical results. As for these patients, they complain of unsatisfactory or no change in their pain relief or even worse pain, which may indicate persistent compression or recurrent fractures in the treated vertebrae. Previous studies have shown that intravertebral vacuum clefting (IVC) in acute OVCF is not an uncommon phenomenon and is also considered an important risk factor for persistent back pain and severe vertebral collapse, which may be the main reason for unsatisfactory outcomes after PKP.
What is balloon kyphoplasty?
Balloon kyphoplasty is a minimally invasive procedure designed to repair vertebral compression fractures (VCF) by reducing and stabilizing fractures. It treats pathological vertebral fractures caused by osteoporosis, cancer or benign lesions.
How Balloon Osteoplasty Works
Creating a space for the balloon
The surgeon will make a pathway into the fractured vertebra using a hollow instrument. A small balloon is then guided through the instrument into the bone.
Inflating the balloon
Once in position, the balloon is slowly inflated to gently raise the collapsed bone into its normal position.
Removing the balloon
When the bone is in the correct position, the surgeon deflates and removes the balloon. This leaves behind a void—or cavity—within the vertebral body.
Filling the vertebral void
To prevent the bone from collapsing again, the void is filled with orthopaedic cement.
Forming the internal cast
Once set, the cement forms a cast inside the vertebral body that stabilizes the bone. To fully secure the bone, the procedure is sometimes performed on both sides of the vertebral body.
The primary benefits of balloon kyphoplasty include:
A shorter surgical time; the procedure usually takes about a half hour per spinal level.
The kyphoplasty procedure can often be performed with local anesthesia. However, some patients, depending on their general health and severity of the spinal fracture(s) may require general anesthesia.
Patients are able to walk and return to their normal activities soon after surgery.
Kyphoplasty may be performed in an ambulatory surgery center (ASC), hospital, or outpatient spine surgery center.
Most patients are discharged home the same day as their kyphoplasty procedure. An overnight hospital stay may be recommended for some patients depending on many factors, such as coexisting medical problems (eg, cardiovascular risks).
Length of Stay and Recovery
Your doctor will give you specific post-operative instructions, but generally, you will spend about an hour in the recovery room after the procedure. There, a nurse diligently monitors your vital signs, which includes back pain.
Most patients are discharged from the ASC or hospital within 24 hours of their balloon kyphoplasty procedure. At your surgical follow-up appointment, your doctor will assess your recovery progress to determine if you should limit certain activities (eg, lifting). Many patients report significant improvements in pain, mobility and the ability to perform daily tasks—so you may not need to make any adjustments to your physical activity level.
Español
Русский
Français
English
العربية
Português
Deutsch
italiano
日本語
한국어
Nederlands
Tiếng Việt
ไทย
Polski
Türkçe
አማርኛ
ພາສາລາວ
ភាសាខ្មែរ
Bahasa Melayu
ဗမာစာ
தமிழ்
Filipino
Bahasa Indonesia
magyar
Română
Čeština
Монгол
қазақ
Српски
हिन्दी
فارسی
Kiswahili
Slovenčina
Slovenščina
Norsk
Svenska
українська
Ελληνικά
Suomi
Հայերեն
עברית
Latine
Dansk
اردو
Shqip
বাংলা
Hrvatski
Afrikaans
Gaeilge
Eesti keel
Māori
नेपाली
Oʻzbekcha
latviešu
অসমীয়া
Aymara
Azərbaycan dili
Bamanankan
Euskara
Беларуская мова
भोजपुरी
Bosanski
Български
Català
Cebuano
Corsu
ދިވެހި
डोग्रिड ने दी
Esperanto
Eʋegbe
Frysk
Galego
ქართული
guarani
ગુજરાતી
Kreyòl ayisyen
Hausa
ʻŌlelo Hawaiʻi
Hmoob
íslenska
Igbo
Ilocano
Basa Jawa
ಕನ್ನಡ
Kinyarwanda
गोंगेन हें नांव
Krio we dɛn kɔl Krio
Kurdî
Kurdî
Кыргызча
Lingala
Lietuvių
Oluganda
Lëtzebuergesch
Македонски
मैथिली
Malagasy
മലയാളം
Malti
मराठी
ꯃꯦꯇꯥꯏ (ꯃꯅꯤꯄꯨꯔꯤ) ꯴.
Mizo tawng
Chichewa
ଓଡ଼ିଆ
Afaan Oromoo
پښتو
ਪੰਜਾਬੀ
Runasimi
Gagana Samoa
संस्कृत
Gaelo Albannach
Sepeti
Sesotho
chiShona
سنڌي
Soomaali
Basa Sunda
Wikang Tagalog
Тоҷикӣ
Татарча
తెలుగు
ትግንያውያን
Xitsonga
Türkmençe
संस्कृत
ئۇيغۇرچە
Cymraeg
isiXhosa
ייִדיש
Yorùbá
isiZulu