Reversed Femoral Nail: A Comprehensive Guide
In orthopedic surgery, femoral fractures are a common occurrence. Femoral nails are frequently used to fix such fractures. The reversed femoral nail is a new and innovative method of fixing fractures, particularly in elderly patients. In this article, we'll discuss everything there is to know about reversed femoral nails, including their benefits, indications, and potential complications.
What is a Reversed Femoral Nail?
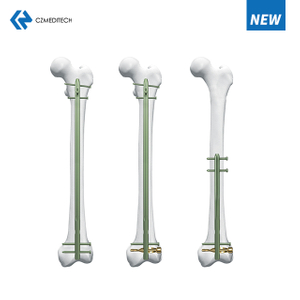
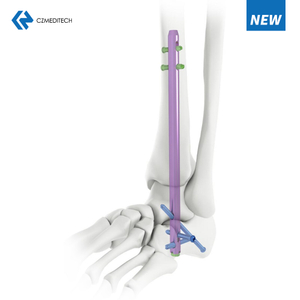
A reversed femoral nail is an orthopedic device used to treat femoral fractures. It is a relatively new technique that involves inserting the nail from the bottom of the femur upwards, which is opposite to the conventional method. The nail is inserted through a small incision in the knee joint and is fixed in place using screws at both ends.
Indications for Reversed Femoral Nails
The reversed femoral nail technique is particularly useful in certain circumstances, such as:
Elderly patients who have fragile bones
Patients with a distal femoral fracture
Patients with a subtrochanteric fracture
Patients with a fracture in the metaphyseal region
In these cases, the reversed femoral nail technique may be a better option than conventional techniques.
Benefits of Reversed Femoral Nails
Reversed femoral nails offer several benefits over conventional techniques. These include:
Reduced blood loss during surgery
Less trauma to the surrounding soft tissues
Less pain and a quicker recovery period
Lower risk of infection
Reduced risk of non-union (a condition in which the bone fails to heal properly)
The Reversed Femoral Nail Procedure
The reversed femoral nail procedure is similar to conventional femoral nail surgery, with a few key differences. The surgery is performed under general anesthesia, and the patient is positioned on their back with their legs elevated.
The surgical team will make a small incision just above the knee joint and insert a guide wire through the knee and up into the femur. The guide wire will be used to guide the nail into place. The nail is then inserted through the knee joint and up into the femur, with screws placed at both ends to hold it in place.
Complications of Reversed Femoral Nails
Like all surgical procedures, reversed femoral nails carry some risks. These include:
Infection at the surgical site
Fracture of the femur during surgery
Nerve damage
Blood vessel damage
Failure of the bone to heal properly
Patients who have undergone a reversed femoral nail procedure should monitor their recovery closely and report any unusual symptoms to their doctor immediately.
Recovery from Reversed Femoral Nails
Recovery from a reversed femoral nail procedure is similar to recovery from conventional femoral nail surgery. Patients may experience some pain and swelling at the surgical site, which can be managed with pain medication and rest. Patients will need to use crutches or a walker for a period of time after surgery to avoid putting weight on the affected leg.
Patients should follow their doctor's instructions carefully to ensure a full and speedy recovery.
Reversed Femoral Nail FAQs
What is the recovery time for a reversed femoral nail procedure?
The recovery time varies depending on the patient and the extent of the surgery, but most patients can expect to return to normal activities within 6-12 weeks.
Is a reversed femoral nail procedure painful?
There may be some pain and discomfort after surgery, but this can be managed with pain medication.
Can anyone have a reversed femoral nail procedure?
No, the reversed femoral nail procedure is not suitable for all patients. Your doctor will assess your individual circumstances to determine if it is the bestoption for you.
How long does the reversed femoral nail stay in place?
The nail is typically left in place for 6-12 months to allow the bone to heal properly.
Can a reversed femoral nail be removed?
Yes, the nail can be removed once the bone has healed. Your doctor will assess whether removal is necessary and discuss the risks and benefits with you.
Conclusion
Reversed femoral nails offer several benefits over conventional techniques for fixing femoral fractures. The technique is particularly useful in elderly patients or those with certain types of fractures. While there are potential complications associated with the procedure, the benefits often outweigh the risks. Patients who have undergone a reversed femoral nail procedure should follow their doctor's instructions carefully to ensure a full and speedy recovery.
In summary, the reversed femoral nail is a new and innovative method of fixing femoral fractures that offers several benefits over conventional techniques. If you are experiencing a femoral fracture, speak to your doctor to determine if the reversed femoral nail technique is right for you.
Español
Русский
Français
English
العربية
Português
Deutsch
italiano
日本語
한국어
Nederlands
Tiếng Việt
ไทย
Polski
Türkçe
አማርኛ
ພາສາລາວ
ភាសាខ្មែរ
Bahasa Melayu
ဗမာစာ
தமிழ்
Filipino
Bahasa Indonesia
magyar
Română
Čeština
Монгол
қазақ
Српски
हिन्दी
فارسی
Kiswahili
Slovenčina
Slovenščina
Norsk
Svenska
українська
Ελληνικά
Suomi
Հայերեն
עברית
Latine
Dansk
اردو
Shqip
বাংলা
Hrvatski
Afrikaans
Gaeilge
Eesti keel
Māori
नेपाली
Oʻzbekcha
latviešu
অসমীয়া
Aymara
Azərbaycan dili
Bamanankan
Euskara
Беларуская мова
भोजपुरी
Bosanski
Български
Català
Cebuano
Corsu
ދިވެހި
डोग्रिड ने दी
Esperanto
Eʋegbe
Frysk
Galego
ქართული
guarani
ગુજરાતી
Kreyòl ayisyen
Hausa
ʻŌlelo Hawaiʻi
Hmoob
íslenska
Igbo
Ilocano
Basa Jawa
ಕನ್ನಡ
Kinyarwanda
गोंगेन हें नांव
Krio we dɛn kɔl Krio
Kurdî
Kurdî
Кыргызча
Lingala
Lietuvių
Oluganda
Lëtzebuergesch
Македонски
मैथिली
Malagasy
മലയാളം
Malti
मराठी
ꯃꯦꯇꯥꯏ (ꯃꯅꯤꯄꯨꯔꯤ) ꯴.
Mizo tawng
Chichewa
ଓଡ଼ିଆ
Afaan Oromoo
پښتو
ਪੰਜਾਬੀ
Runasimi
Gagana Samoa
संस्कृत
Gaelo Albannach
Sepeti
Sesotho
chiShona
سنڌي
Soomaali
Basa Sunda
Wikang Tagalog
Тоҷикӣ
Татарча
తెలుగు
ትግንያውያን
Xitsonga
Türkmençe
संस्कृत
ئۇيغۇرچە
Cymraeg
isiXhosa
ייִדיש
Yorùbá
isiZulu