What Are Cervical Implants?
Cervical implants are specialized medical devices used in cervical spine surgery to restore spinal stability, maintain alignment, and relieve neurological symptoms caused by cervical spine disorders. These implants play a critical role in treating degenerative, traumatic, and deformity-related conditions of the neck while improving patient mobility and quality of life.
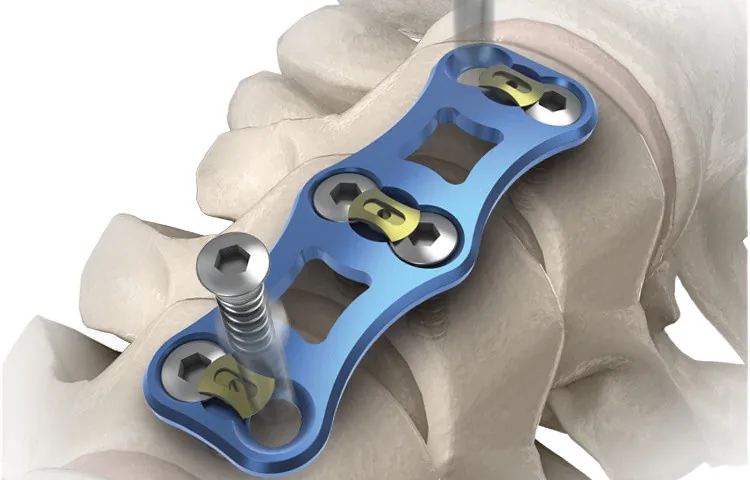
Overview of Cervical Spine Implants
Cervical spine implants are designed to support, replace, or stabilize components of the cervical vertebrae following surgical intervention. They are commonly used when conservative treatments fail to relieve pain, neurological deficits, or mechanical instability.
From a clinical perspective, cervical implants help surgeons achieve spinal decompression, fusion, or motion preservation depending on the selected procedure. Modern cervical implant systems emphasize biomechanical stability, biocompatibility, and long-term clinical reliability.
Anatomy of the Cervical Spine and Its Clinical Significance
The cervical spine consists of seven vertebrae (C1–C7) located at the top of the spinal column. This region supports the head, protects the spinal cord, and allows for a wide range of motion.
Cervical Vertebrae C1–C7 and Functional Roles
Each cervical vertebra contributes differently to neck movement and load distribution. The upper cervical spine (C1–C2) is primarily responsible for rotation, while the lower cervical segments (C3–C7) facilitate flexion, extension, and lateral bending.
Intervertebral Discs, Spinal Cord, and Nerve Roots
Between the vertebrae lie intervertebral discs that absorb shock and maintain spacing for nerve roots. Degeneration or injury in this area can compress neural structures, often necessitating surgical intervention with cervical implants.
Why Cervical Spinal Implants Are Required
Cervical implants are typically indicated when structural damage or degeneration compromises spinal stability or neurological function.
Degenerative Cervical Disc Disease and Herniation
Age-related disc degeneration or disc herniation can cause chronic neck pain, radiculopathy, or myelopathy. Cervical implants help restore disc height and relieve nerve compression.
Cervical Spinal Stenosis and Neurological Compression
Narrowing of the spinal canal may compress the spinal cord or nerve roots, leading to weakness, numbness, or gait disturbances. Surgical decompression often requires stabilization with implants.
Cervical Fractures and Instability
Traumatic injuries can disrupt spinal alignment. Cervical fixation systems are essential to restore mechanical stability and prevent secondary neurological injury.
![Posterior-Cervical-Vertebra-Fixation-Pedicle-Screw_副本_副本]()
Types of Cervical Implants Used in Spine Surgery
Different cervical implant systems are selected based on pathology, surgical approach, and desired clinical outcome.
Anterior Cervical Plate Systems for ACDF
Anterior cervical plates are commonly used in anterior cervical discectomy and fusion (ACDF) procedures. These plates provide immediate stability and promote successful bone fusion between vertebral bodies.
Cervical Disc Replacement and Motion Preservation Devices
Artificial cervical discs are designed to preserve physiological motion while alleviating pain caused by disc degeneration. Cervical disc replacement is often considered for younger or more active patients.
Posterior Cervical Fixation Systems
Posterior cervical screws and rods are used to stabilize the spine from the back of the neck, particularly in multi-level fusion or complex deformity cases.
Corpectomy Cages and Structural Support Implants
In cases involving vertebral body removal, corpectomy cages provide anterior column support and help maintain spinal alignment.
Cervical Implant Materials and Design Considerations
Material selection plays a crucial role in implant performance and long-term outcomes.
Titanium and Titanium Alloy Cervical Implants
Titanium implants offer excellent strength, corrosion resistance, and osseointegration, making them widely used in cervical fixation systems.
PEEK Cervical Cages and Radiolucent Benefits
PEEK (polyetheretherketone) cages provide elastic modulus closer to bone and allow for clearer postoperative imaging, supporting accurate fusion assessment.
Advanced Surface Treatments and 3D-Printed Implants
Modern cervical implants may feature porous structures or 3D-printed designs to enhance bone integration and biomechanical compatibility.
Cervical Implant Surgical Procedures and Approaches
Cervical implant surgery is carefully planned based on patient anatomy and pathology.
Preoperative Evaluation and Surgical Planning
Imaging studies such as MRI and CT scans are used to assess spinal alignment, neural compression, and bone quality before selecting the appropriate implant system.
Anterior Cervical Surgery Techniques
Anterior approaches are commonly used for disc replacement and fusion procedures, allowing direct access to the cervical discs with minimal muscle disruption.
Posterior Cervical Surgery Techniques
Posterior approaches are preferred in cases requiring extensive decompression or multi-level stabilization.
Recovery and Rehabilitation After Cervical Implant Surgery
Postoperative recovery varies depending on the procedure and patient condition.
Early Postoperative Care and Cervical Bracing
Some patients may require a cervical collar to limit movement and support healing during the early recovery phase.
Physical Therapy and Functional Rehabilitation
Rehabilitation programs focus on restoring neck mobility, strengthening surrounding muscles, and improving overall function.
Long-Term Outcomes and Activity Resumption
Most patients experience significant symptom improvement, with gradual return to daily activities under medical guidance.
Risks, Complications, and Long-Term Safety of Cervical Implants
While cervical implant surgery is generally safe, potential risks should be understood.
Implant Loosening, Infection, and Hardware Failure
Proper surgical technique and postoperative care reduce the risk of implant-related complications.
Adjacent Segment Degeneration and Revision Surgery
Fusion procedures may increase stress on adjacent segments, occasionally requiring further intervention.
How to Choose the Appropriate Cervical Implant System
Selecting the optimal cervical implant involves multiple factors.
Patient Anatomy and Bone Quality Considerations
Age, bone density, and spinal alignment influence implant selection.
Fusion Versus Motion Preservation Strategies
Surgeons weigh the benefits of stability against the desire to maintain natural cervical motion.
Regulatory Standards and Surgeon Experience
Implants should meet international regulatory requirements and be supported by clinical evidence.
Conclusion: The Role of Cervical Implants in Modern Spine Surgery
Cervical implants are essential tools in the treatment of cervical spine disorders, providing stability, pain relief, and improved neurological outcomes. With advances in implant design, materials, and surgical techniques, cervical spine surgery continues to deliver reliable and predictable results for patients worldwide.
For surgeons and medical device buyers, understanding cervical implant options is key to achieving optimal clinical outcomes and long-term success.
Cervical spinal implants are medical devices that are surgically implanted in the neck to provide stability and support to the cervical spine. They are used to treat a variety of conditions, including degenerative disc disease, spinal stenosis, and herniated discs. In this article, we will discuss the different types of cervical spinal implants, their uses, and the surgical procedures involved.
FAQ 0f cervical implants
What are cervical implants used for?
Cervical implants are used to stabilize the cervical spine, relieve nerve compression, restore alignment, and support fusion or motion preservation after cervical spine surgery.
What conditions require cervical implant surgery?
Cervical implant surgery is commonly performed for degenerative disc disease, cervical disc herniation, spinal stenosis, fractures, instability, and spinal cord compression.
What are the main types of cervical spine implants?
The most common cervical implants include anterior cervical plates, cervical disc replacement devices, posterior fixation systems, and corpectomy cages.
What materials are used in cervical implants?
Cervical implants are typically made from titanium alloys or PEEK materials, chosen for their strength, biocompatibility, and compatibility with spinal fusion or motion preservation.
What is the difference between cervical fusion and disc replacement?
Cervical fusion eliminates motion at the treated segment to provide stability, while cervical disc replacement preserves natural motion and may reduce stress on adjacent segments.
How long does recovery take after cervical implant surgery?
Recovery time varies by procedure, but most patients resume normal daily activities within weeks, with full recovery and fusion assessment taking several months.
Are cervical implants safe for long-term use?
Modern cervical implants are designed for long-term safety and durability, with high clinical success rates when properly selected and surgically implanted.
Can cervical implants be removed or revised?
In rare cases involving complications or adjacent segment disease, cervical implants may require revision or removal, depending on clinical evaluation.
![czmeditech-Request a Quote-CTA czmeditech-Request a Quote-CTA]()
Español
Русский
Français
English
العربية
Português
Deutsch
italiano
日本語
한국어
Nederlands
Tiếng Việt
ไทย
Polski
Türkçe
አማርኛ
ພາສາລາວ
ភាសាខ្មែរ
Bahasa Melayu
ဗမာစာ
தமிழ்
Filipino
Bahasa Indonesia
magyar
Română
Čeština
Монгол
қазақ
Српски
हिन्दी
فارسی
Kiswahili
Slovenčina
Slovenščina
Norsk
Svenska
українська
Ελληνικά
Suomi
Հայերեն
עברית
Latine
Dansk
اردو
Shqip
বাংলা
Hrvatski
Afrikaans
Gaeilge
Eesti keel
Māori
नेपाली
Oʻzbekcha
latviešu
অসমীয়া
Aymara
Azərbaycan dili
Bamanankan
Euskara
Беларуская мова
भोजपुरी
Bosanski
Български
Català
Cebuano
Corsu
ދިވެހި
डोग्रिड ने दी
Esperanto
Eʋegbe
Frysk
Galego
ქართული
guarani
ગુજરાતી
Kreyòl ayisyen
Hausa
ʻŌlelo Hawaiʻi
Hmoob
íslenska
Igbo
Ilocano
Basa Jawa
ಕನ್ನಡ
Kinyarwanda
गोंगेन हें नांव
Krio we dɛn kɔl Krio
Kurdî
Kurdî
Кыргызча
Lingala
Lietuvių
Oluganda
Lëtzebuergesch
Македонски
मैथिली
Malagasy
മലയാളം
Malti
मराठी
ꯃꯦꯇꯥꯏ (ꯃꯅꯤꯄꯨꯔꯤ) ꯴.
Mizo tawng
Chichewa
ଓଡ଼ିଆ
Afaan Oromoo
پښتو
ਪੰਜਾਬੀ
Runasimi
Gagana Samoa
संस्कृत
Gaelo Albannach
Sepeti
Sesotho
chiShona
سنڌي
Soomaali
Basa Sunda
Wikang Tagalog
Тоҷикӣ
Татарча
తెలుగు
ትግንያውያን
Xitsonga
Türkmençe
संस्कृत
ئۇيغۇرچە
Cymraeg
isiXhosa
ייִדיש
Yorùbá
isiZulu













