What Are Spinal Implants — Definition, Purpose and Clinical Role
Spinal implants are specialized medical devices designed to support, stabilize, or restore the structural integrity of the spine. They are widely used in modern spinal surgery to treat a variety of degenerative, traumatic, and deformity-related spinal conditions.
Rather than replacing biological tissue, most spinal implants work in conjunction with the patient’s anatomy to maintain alignment, promote fusion, and reduce mechanical stress on affected spinal segments.
Spinal Implant Definition and Functional Overview
From a clinical perspective, spinal implants include fixation devices, interbody support systems, and motion-preserving components that are surgically placed within or adjacent to the spinal column. Their primary function is to control spinal motion while healing occurs or to permanently stabilize unstable spinal segments.
These implants are engineered to withstand complex biomechanical loads, including axial compression, bending, and torsional forces generated during daily movement.
Key Clinical Purposes: Stability, Alignment and Pain Relief
The main clinical objectives of spinal implants include restoring spinal stability, maintaining physiological alignment, and relieving nerve compression. By limiting abnormal motion between vertebrae, implants help reduce pain caused by instability or degenerative changes.
In many cases, spinal implants also create an optimal environment for bone fusion, allowing vertebrae to gradually fuse into a single stable unit.
Biocompatible Materials and Implant Engineering
Modern spinal implants are manufactured from biocompatible materials such as titanium alloys, PEEK (polyetheretherketone), and, in some cases, carbon fiber–reinforced polymers. These materials are selected for their strength, corrosion resistance, imaging compatibility, and long-term biological safety.
Material selection plays a critical role in implant performance, particularly in load sharing, osseointegration, and postoperative imaging clarity.
Types of Spinal Implants — Classification and Use Cases
Spinal implants can be broadly classified based on their anatomical location, fixation method, and surgical purpose. Each category serves a specific role in spinal reconstruction or stabilization.
Pedicle Screws and Rod Systems for Spinal Stabilization
Pedicle screw and rod systems are among the most commonly used spinal fixation devices. Pedicle screws are inserted into the vertebral pedicles and connected with rods to stabilize one or more spinal segments.
These systems are widely applied in spinal fusion surgery, trauma stabilization, and deformity correction due to their strong fixation strength and adaptability.
Interbody Fusion Cages — Lumbar, Cervical and Thoracic Applications
Interbody fusion cages are implanted between adjacent vertebral bodies after disc removal. Their primary function is to restore disc height, maintain foraminal space, and facilitate bone fusion.
Depending on the surgical approach, interbody cages are used in cervical, thoracic, and lumbar procedures, with designs optimized for anatomical fit and load distribution.
Plates, Hooks and Auxiliary Fixation Devices
Spinal plates, hooks, and auxiliary fixation components provide additional stability in specific anatomical regions, particularly in cervical and upper thoracic surgeries. These devices are often used in combination with screws and rods to enhance fixation strength and alignment control.
Motion-Preserving Devices and Non-Fusion Implants
Not all spinal conditions require rigid fusion. Motion-preserving spinal implants, such as artificial discs and dynamic stabilization systems, aim to maintain controlled spinal mobility while reducing pain and degeneration.
These systems are typically selected for carefully evaluated patients where preserving segmental motion is clinically advantageous.
![Types of Spinal Implants — Classification and Use Cases]()
Spinal Conditions That Require Implant Surgery
Spinal implants are indicated for a wide range of pathological conditions where conservative treatment is insufficient or structural instability is present.
Degenerative Disc Disease and Spinal Instability
Degenerative disc disease can lead to disc collapse, abnormal motion, and chronic pain. When instability becomes significant, spinal implants are used to restore alignment and mechanical stability, often in combination with fusion procedures.
Spinal Fractures and Trauma Stabilization
Traumatic spinal fractures resulting from accidents or falls may compromise spinal stability and neurological safety. Implant-based fixation allows surgeons to realign fractured segments and protect the spinal cord during healing.
Scoliosis, Kyphosis and Spinal Deformity Correction
In spinal deformities such as scoliosis and kyphosis, implants play a critical role in gradual deformity correction and long-term stabilization. Multi-level fixation systems help restore balanced spinal alignment and prevent progression.
Spondylolisthesis, Herniated Discs and Nerve Compression
Conditions involving vertebral slippage or disc herniation may lead to nerve compression and functional impairment. Spinal implants assist in decompression procedures by maintaining corrected alignment and preventing recurrent instability.
Surgical Techniques and Implant Placement Procedures
The success of spinal implants depends not only on implant design but also on precise surgical planning and execution.
Pre-operative Evaluation and Imaging Assessment
Preoperative evaluation typically includes X-ray, CT, and MRI imaging to assess spinal anatomy, instability, and neural structures. Accurate imaging guides implant selection, sizing, and surgical approach.
Spinal Fusion Surgery vs Minimally Invasive Techniques
Traditional open spinal fusion remains widely used, but minimally invasive spinal surgery techniques have gained popularity due to reduced tissue damage and faster recovery. Both approaches utilize spinal implants, with differences primarily in surgical access and instrumentation.
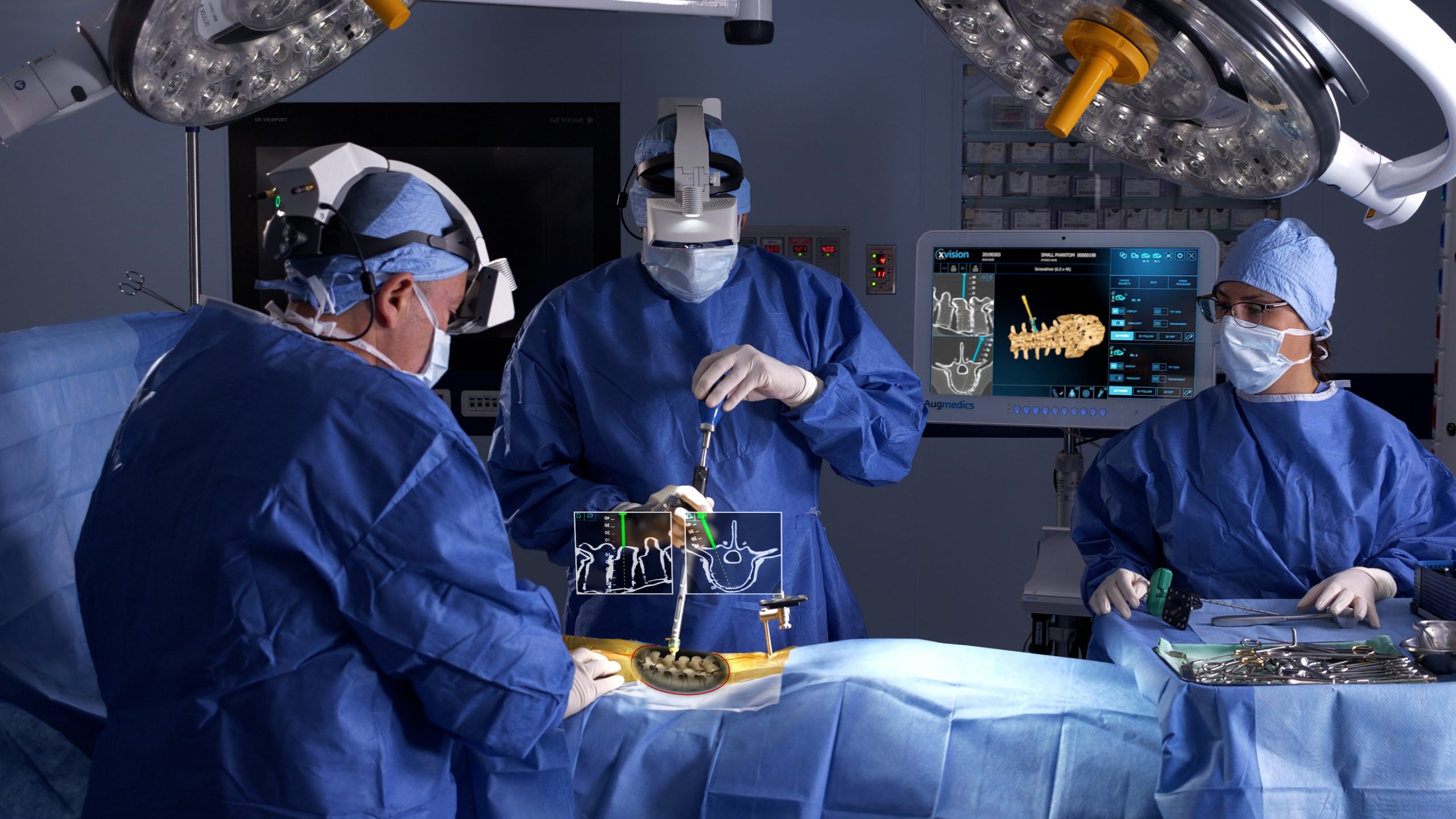
Intraoperative Navigation and Precision Placement
Advanced intraoperative navigation systems and robotic assistance improve the accuracy of implant placement. Precise positioning reduces the risk of complications and enhances biomechanical performance.
Recovery, Rehabilitation and Long-Term Follow-Up
Postoperative recovery includes structured rehabilitation to restore mobility and strength. Long-term follow-up is essential to monitor fusion progress, implant stability, and functional outcomes.
![Surgical Procedure for Spinal Implants]()
Benefits of Spinal Implants — Clinical Outcomes and Patient Impact
When appropriately selected and properly implanted, spinal implants offer significant clinical benefits.
Pain Relief and Functional Improvement
By stabilizing unstable segments and relieving nerve compression, spinal implants contribute to substantial pain reduction and improved daily function for many patients.
Enhanced Spinal Stability and Load Distribution
Implants redistribute mechanical loads across the spine, reducing stress on damaged structures and preventing further degeneration or deformity progression.
Quality of Life and Return to Activity
Improved spinal stability and pain control enable patients to return to normal activities and achieve better long-term quality of life.
Risks, Complications and Post-Operative Considerations
As with any surgical intervention, spinal implant procedures carry potential risks that must be carefully managed.
Infection Control and Wound Management
Strict surgical protocols and postoperative care are essential to minimize infection risk. Early detection and intervention are critical for successful outcomes.
Implant Failure, Loosening and Revision Surgery
Implant-related complications may include loosening, breakage, or non-union. These issues may require revision surgery depending on clinical severity.
Neurological Risks and Safety Protocols
Meticulous surgical technique and intraoperative monitoring are used to reduce the risk of neurological injury during implant placement.
Innovations and Future Trends in Spinal Implants
Spinal implant technology continues to evolve alongside advances in materials science and surgical techniques.
3D-Printed and Patient-Specific Spinal Implants
Additive manufacturing enables patient-specific implant designs tailored to individual anatomy, improving fit and biomechanical compatibility.
Motion-Preservation Systems and Dynamic Stabilization
Next-generation motion-preserving systems aim to balance stability with controlled mobility, addressing limitations of traditional fusion approaches.
Robotics, Navigation and AI-Assisted Spine Surgery
Robotics and AI-driven navigation systems are increasingly integrated into spinal surgery, enhancing precision, consistency, and long-term outcomes.
Conclusion
Spinal implants are a cornerstone of modern spinal surgery, offering reliable solutions for stabilization, alignment, and pain relief across a wide range of spinal conditions. As implant technology and surgical techniques continue to advance, spinal implants will play an increasingly important role in improving patient outcomes worldwide.
Español
Русский
Français
English
العربية
Português
Deutsch
italiano
日本語
한국어
Nederlands
Tiếng Việt
ไทย
Polski
Türkçe
አማርኛ
ພາສາລາວ
ភាសាខ្មែរ
Bahasa Melayu
ဗမာစာ
தமிழ்
Filipino
Bahasa Indonesia
magyar
Română
Čeština
Монгол
қазақ
Српски
हिन्दी
فارسی
Kiswahili
Slovenčina
Slovenščina
Norsk
Svenska
українська
Ελληνικά
Suomi
Հայերեն
עברית
Latine
Dansk
اردو
Shqip
বাংলা
Hrvatski
Afrikaans
Gaeilge
Eesti keel
Māori
नेपाली
Oʻzbekcha
latviešu
অসমীয়া
Aymara
Azərbaycan dili
Bamanankan
Euskara
Беларуская мова
भोजपुरी
Bosanski
Български
Català
Cebuano
Corsu
ދިވެހި
डोग्रिड ने दी
Esperanto
Eʋegbe
Frysk
Galego
ქართული
guarani
ગુજરાતી
Kreyòl ayisyen
Hausa
ʻŌlelo Hawaiʻi
Hmoob
íslenska
Igbo
Ilocano
Basa Jawa
ಕನ್ನಡ
Kinyarwanda
गोंगेन हें नांव
Krio we dɛn kɔl Krio
Kurdî
Kurdî
Кыргызча
Lingala
Lietuvių
Oluganda
Lëtzebuergesch
Македонски
मैथिली
Malagasy
മലയാളം
Malti
मराठी
ꯃꯦꯇꯥꯏ (ꯃꯅꯤꯄꯨꯔꯤ) ꯴.
Mizo tawng
Chichewa
ଓଡ଼ିଆ
Afaan Oromoo
پښتو
ਪੰਜਾਬੀ
Runasimi
Gagana Samoa
संस्कृत
Gaelo Albannach
Sepeti
Sesotho
chiShona
سنڌي
Soomaali
Basa Sunda
Wikang Tagalog
Тоҷикӣ
Татарча
తెలుగు
ትግንያውያን
Xitsonga
Türkmençe
संस्कृत
ئۇيغۇرچە
Cymraeg
isiXhosa
ייִדיש
Yorùbá
isiZulu